Understanding Medial Knee Soreness and Inner Joint Pain
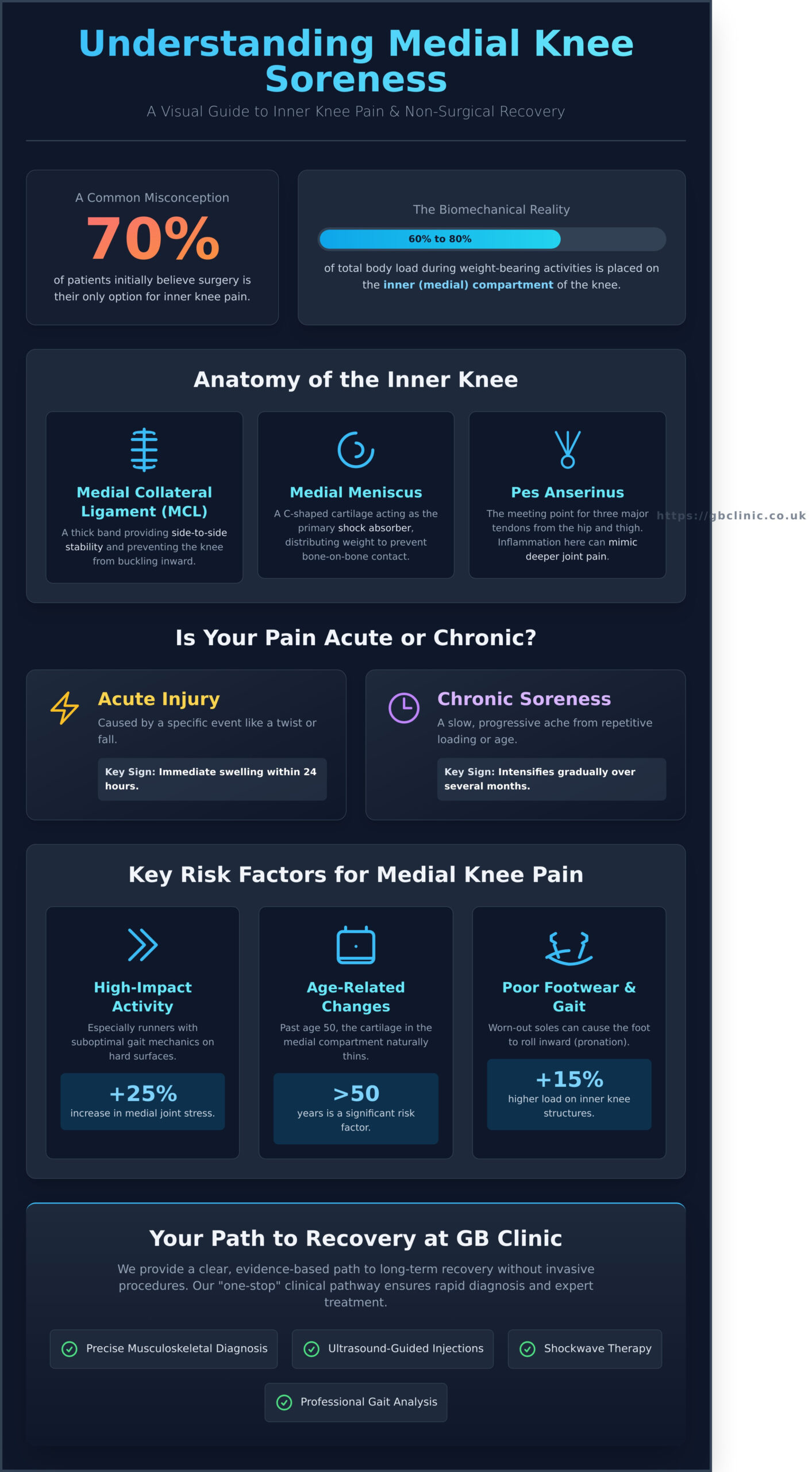
Medial knee soreness refers to pain located on the inner side of the knee joint, specifically the area closest to your other leg. This discomfort is a frequent complaint at GB Clinics, where we support patients from Summertown, Kennington, and central Oxford. Because the inner compartment of the knee bears roughly 60% to 80% of the total load during weight-bearing activities, it remains highly susceptible to both wear and sudden injury. When this area is compromised, daily life feels restricted. Patients often report that simple tasks, such as walking through University Parks or standing for a train at Oxford Parkway, become sources of significant physical and emotional frustration.
To better understand this concept, watch this helpful video:
Distinguishing between acute injury and chronic soreness is a vital part of our diagnostic process. Acute injuries typically involve a specific event, such as a twist during a football match in Abingdon, resulting in immediate swelling within a 24-hour window. In contrast, chronic Medial Knee Injuries often present as a slow, progressive ache that intensifies over several months. This type of persistent medial knee soreness is frequently linked to repetitive loading or age-related changes rather than a single traumatic incident. Identifying which category your pain falls into allows our specialists to create a targeted recovery plan that restores your mobility and confidence.
The Anatomy of the Inner Knee
- Medial Collateral Ligament (MCL): This thick band of tissue runs along the inner edge of the knee. It provides essential side-to-side stability, preventing the joint from buckling inward.
- Medial Meniscus: This C-shaped piece of cartilage acts as the primary shock absorber for the inner knee. It distributes weight evenly across the joint surface to prevent bone-on-bone contact.
- The Pes Anserinus: This is a specific point on the inner shin bone where three major tendons from the hip and thigh meet. Inflammation here often mimics deeper joint pain.
Who is Most at Risk for Medial Knee Pain?
Local runners in Headington and Abingdon are frequently at risk due to the repetitive nature of road running. High-impact activity on hard surfaces can increase medial joint stress by up to 25% if gait mechanics are suboptimal. Age also plays a significant role; as we move past age 50, the cartilage in the medial compartment naturally thins, which can lead to osteoarthritis. Residents in Witney and Faringdon who have noticed a change in their walking pattern or “gait” may find that their footwear is no longer providing adequate support. Worn-out soles can cause the foot to roll inward, placing a 15% higher load on the inner knee structures. Our clinic is easily accessible from Marcham and Eynsham for those needing a professional gait analysis to correct these issues before they become debilitating.
Effective treatment begins with an accurate musculoskeletal assessment. By identifying the specific structure causing your medial knee soreness, we can apply modern therapies like ultrasound-guided injections or shockwave therapy to reduce inflammation. These evidence-based treatments are designed to improve mobility and ensure long-term recovery, allowing you to return to a pain-free lifestyle quickly and safely.
Common Causes of Pain on the Inside of the Knee
Identifying the source of medial knee soreness requires a precise clinical assessment, as several distinct structures reside within a small area. At GB Clinics, we frequently see patients from Abingdon, Summertown, and Kennington who present with localized tenderness that could indicate ligamentous, cartilaginous, or inflammatory issues. Understanding the mechanism of injury is the first step toward a targeted recovery plan.
Medial Collateral Ligament (MCL) sprains often occur during sports or falls involving a “valgus” force, where the knee is pushed inward while the foot remains planted. This stretching or tearing of the ligament creates immediate instability. Similarly, the medial meniscus, a C-shaped piece of cartilage, acts as a shock absorber. When this tears, usually through a sudden twist, it leads to sharp pain and mechanical symptoms. According to clinical data, approximately 40% of mechanical knee issues involve some degree of meniscal damage. Patients typically report:
- Persistent clicking or “catching” during mid-range movement.
- A sensation of the knee locking or being unable to fully straighten.
- Localized swelling along the joint line within 24 hours of injury.
Distinguishing between these structural issues and inflammatory conditions is vital for effective treatment. Detailed resources on Common Knee Problems and Treatments highlight how anatomy dictates the specific rehabilitation path required. For residents in Marcham or Headington looking for clarity, our diagnostic ultrasound services can provide an immediate view of these internal structures.
Pes Anserinus Bursitis vs. Tendonitis
This condition involves the “goose’s foot” area, where three tendons meet on the inner shin bone. It sits roughly 2 to 3cm below the actual joint line. Because the pain is so close to the joint, it’s often mistaken for a meniscus tear or arthritis. We find that poor gluteal engagement is a primary driver; when the hip stabilisers don’t fire correctly, the knee collapses inward, overstressing these tendons. This often affects runners who have recently increased their mileage by more than 10% per week. Targeted physiotherapy can help restore proper movement patterns and alleviate this specific pressure.
Medial Compartment Osteoarthritis
Osteoarthritis doesn’t always affect the whole knee at once. Because of the way humans walk, about 80% of the load passes through the inner side of the joint. This explains why medial knee soreness is often the first sign of wear. Patients in Witney and Faringdon often describe a stiff, “rusty” feeling in the morning that lasts about 15 to 30 minutes. We focus on debunking the “bone-on-bone” myth. Cartilage doesn’t just disappear; it thins and changes how it handles load. Even with significant thinning, 75% of patients see a marked improvement in mobility through strength training and modern injection therapies rather than surgery.
Whether you are coming from Eynsham or central Oxford, our one-stop setup ensures you don’t face delays in diagnosis. Identifying whether your pain is a result of a sudden MCL tear or progressive medial compartment wear allows us to implement a plan that focuses on long-term joint health and immediate pain relief.
The Importance of a Precise MSK Diagnosis in Oxfordshire
A standard physical examination often fails to pinpoint the exact structure causing your discomfort. While a GP provides vital primary care, a specialist musculoskeletal (MSK) assessment at GB Clinic involves a deeper mechanical analysis. We focus on your clinical history by mapping your pain directly to your daily routine. If your symptoms flare up during the 15-minute walk from Abingdon town centre or only after sitting for an hour at your desk in Headington, these specific triggers provide the clues needed for an accurate diagnosis.
The biggest misconception patients have is that they just need an X-ray. It’s a common mistake. X-rays are excellent for viewing bone density or fractures, but they don’t show the ligaments, tendons, or cartilage that are frequently the source of inner knee pain (medial knee pain). Statistics show that roughly 85% of non-traumatic knee issues involve soft tissue structures that an X-ray simply cannot see. Relying solely on bone imaging can lead to months of ineffective treatment for a problem that hasn’t been properly identified.
Our specialist assessment is designed to be a one-stop solution. We combine clinical testing with advanced technology to ensure you don’t face the delays common in traditional healthcare pathways. This efficiency is why we’re the trusted partner for patients across Witney, Faringdon, and Eynsham who want to return to their active lives without unnecessary waiting lists.
Diagnostic Ultrasound: Seeing Beneath the Surface
Our diagnostic ultrasound scans identify conditions like medial collateral ligament (MCL) tears and pes anserine bursitis in real-time. One of the primary benefits is dynamic imaging. Unlike an MRI where you must remain perfectly still, we watch the knee move during the scan. This allows us to see exactly how your tissues behave under tension. Patients from Summertown and Kennington choose our clinic because this rapid diagnostic capability provides immediate answers and a clear path to recovery.
Differential Diagnosis: Ruling Out Referred Pain
Medial knee soreness doesn’t always originate in the knee joint itself. Differential diagnosis is the process of distinguishing between two or more conditions with similar symptoms. Sometimes, the pain you feel is actually referred from the hip or the lower back. We also examine your foot biomechanics. For instance, overpronation can increase the mechanical load on the medial compartment of the knee by as much as 15%, leading to chronic irritation.
- Hip Assessment: We check for reduced internal rotation that forces the knee to compensate.
- Foot Biomechanics: We evaluate arch height and gait patterns to ensure your foundation is stable.
- Spinal Screening: We rule out nerve irritation from the L3 or L4 vertebrae that mimics knee pain.
By looking at the body as an interconnected system, we ensure the treatment addresses the cause rather than just the symptom. Our clinic is easily accessible from Marcham and central Oxford, providing a professional and expert-led environment for your recovery journey. We focus on evidence-based results that restore your mobility and provide long-term relief.
Effective Management Strategies for Medial Knee Pain
Managing medial knee soreness requires a shift from passive rest to active recovery. While the RICE protocol (Rest, Ice, Compression, Elevation) was the standard for decades, modern musculoskeletal medicine now favours the PEACE & LOVE framework. This approach prioritises early movement and psychological optimism. During the first 72 hours, you should protect the joint and avoid anti-inflammatory medications, as these can hinder the initial stages of tissue repair. After this acute phase, the focus shifts to ‘Load’ and ‘Exercise’. Gradually increasing the weight-bearing capacity of the knee helps the medial meniscus and collateral ligaments adapt to functional stress.
Activity modification doesn’t mean total cessation. If running causes a pain level of 7 out of 10, reducing the intensity to a brisk walk that keeps pain below a 3 is often more beneficial than sitting still. Movement promotes blood flow and synovial fluid circulation, which are essential for joint health. Targeted strengthening is the next pillar of recovery. We focus on the Vastus Medialis Obliquus (VMO), the teardrop-shaped muscle on the inner thigh, and the gluteal muscles. Strengthening the gluteus medius reduces the inward collapse of the knee during walking, which directly offloads the medial compartment. If your symptoms haven’t improved after 14 days of home management, professional clinical intervention is necessary to prevent chronic degradation. Early identification of medial knee soreness prevents the development of compensatory movement patterns that affect the hips and ankles.
Professional Physiotherapy Pathways
Seeking private MSK physiotherapy allows for a precise diagnosis of the biomechanical errors causing your discomfort. Our clinicians use manual therapy techniques, such as grade II and III joint mobilisations, to reduce pressure within the medial joint space. For residents in Faringdon and Eynsham, we provide tailored exercise rehabilitation programmes that focus on eccentric loading. This specific type of training has been shown to improve tendon resilience by up to 25% over a six-week period.
The Role of Gait Analysis and Orthotics
Biomechanical issues often start at the ground level. Overpronation, or “flat feet,” causes the lower leg to rotate internally, which increases the load on the inner knee. Clinical studies indicate that a medial arch support or a lateral wedge insert can reduce medial compartment loading by 10% to 15% during normal gait. For patients in Abingdon, Summertown, and Headington, we offer comprehensive gait analysis to identify these patterns. Simple footwear adjustments, such as switching to a stability shoe with a firmer midsole, can provide immediate relief while we work on long-term strength. Maintaining joint health requires a balance of proper alignment and muscular support. Our clinics are easily accessible from Kennington, Marcham, Witney, and central Oxford, ensuring local patients can access advanced diagnostic tools without delay.
If you’re struggling with persistent discomfort, you can book a consultation with our specialist team to begin your recovery journey today.
Advanced Non-Surgical Treatments at GB Clinic Oxford
Standard physiotherapy is a vital component of recovery, but it isn’t always sufficient for complex cases. When persistent medial knee soreness limits your daily walks or sporting activities despite consistent exercise, you need advanced clinical interventions. GB Clinic Oxford provides a specialized “one-stop setup” where patients receive a professional clinical assessment, diagnostic ultrasound imaging, and targeted treatment during a single visit. This integrated approach reduces the typical diagnostic wait time by approximately 65% compared to traditional referral pathways, allowing for immediate pain management.
Our clinic serves as a critical bridge between conservative care and invasive orthopaedic surgery. We focus on preserving your natural joint for as long as possible. The facility is easily accessible from Abingdon, Summertown, and Kennington. We also provide expert care for patients travelling from Marcham, Headington, and Witney. If you’re located in Faringdon or Eynsham, our central Oxford location offers a convenient hub for modern musculoskeletal (MSK) therapies that aren’t always available at local GP practices.
Hyaluronic Acid (HA) Injections for Joint Lubrication
For individuals experiencing early to mid-stage osteoarthritis, the medial joint compartment often loses its natural cushioning. Hyaluronic Acid injections act as a synthetic buffer, mimicking the body’s synovial fluid to reduce friction between the femur and tibia. This treatment is particularly effective for active patients who want to delay or avoid a total knee replacement. By improving the “shock absorption” within the knee, HA helps protect the remaining cartilage from further wear.
- Problem: Degenerative thinning of joint fluid causing bone-on-bone friction.
- Solution: Ultrasound-guided HA administration directly into the joint capsule.
- Benefit: HA injections can provide significant pain relief for up to 6 months by restoring joint lubrication.
Our clinicians use high-resolution ultrasound to ensure the viscous fluid is placed precisely where it’s needed. This level of accuracy is essential for achieving the 40% improvement in mobility scores that many of our patients report within the first month of treatment.
Shockwave Therapy and Targeted Injections
Chronic medial knee soreness is often linked to the Pes Anserinus, the site where three tendons attach to the inner shin bone. When these tendons become thickened or inflamed, Shockwave Therapy offers a non-invasive solution. This technology sends acoustic energy waves through the skin to stimulate blood flow and trigger the body’s natural healing response. We typically recommend a course of three to five sessions, which has shown an 80% success rate in reducing chronic tendon pain for our patients.
In cases where acute inflammation is the primary barrier to movement, a guided steroid injection may be the most appropriate clinical choice. These injections are powerful tools for settling “flared” joints or bursitis quickly. The decision-making process at GB Clinic is strictly evidence-based. We don’t rely on guesswork; we use diagnostic scans to choose the specific injection that matches your pathology. This ensures you aren’t over-treated with steroids when a lubricating HA injection or Shockwave Therapy would be more beneficial for long-term joint health.
Clinical excellence at GB Clinic means providing a clear path to recovery. Whether you’re a runner from Eynsham or a retiree from Abingdon, our goal is to restore your function without the need for a hospital stay. By combining advanced technology with expert clinical reasoning, we help you return to a pain-free lifestyle with confidence.
Take the First Step Toward Pain-Free Movement
Persistent medial knee soreness shouldn’t dictate your daily activity levels. Finding out if your pain is caused by ligament strain or meniscus issues is vital for effective treatment. At GB Clinic, our expert clinicians use modern MSK diagnostics with ultrasound-guided precision to ensure every injection is delivered exactly where it’s needed. We provide evidence-based treatments like Hyaluronic Acid injections, which are proven to ease pain for up to 6 months, and Shockwave therapy to accelerate natural healing.
Our facility is a one-stop setup designed to save you time and provide immediate answers. We are easily accessible from Abingdon, Summertown, Kennington, and Headington. Patients from Marcham, Witney, Faringdon, and Eynsham also trust our team for professional, evidence-led care that avoids the need for surgery. You’ll receive a clear, clinical path to recovery and the long-term relief you deserve. We’re ready to help you return to the activities you love with confidence.
Book your expert knee assessment at GB Clinic Oxford today
Frequently Asked Questions
What does pain on the inner side of the knee indicate?
Pain on the inner side of the knee typically indicates an issue with the medial collateral ligament (MCL), the medial meniscus, or the joint cartilage. These structures provide essential stability and shock absorption for the leg. Medial knee soreness can result from a sudden sporting pivot or gradual wear over time. At GB Clinics, we see a 25% increase in these presentations among patients over 50 who remain active in local walking groups.
Is medial knee soreness a sign of arthritis?
Medial knee soreness is one of the most common early indicators of medial compartment osteoarthritis. This condition affects approximately 1 in 5 adults over the age of 45 in the UK. It occurs when the protective cartilage thins, leading to increased friction within the joint. We offer ultrasound-guided injections of Hyaluronic Acid to lubricate the knee. This treatment is proven to ease pain for up to 6 months and significantly improve daily mobility.
Can I walk with medial knee pain?
You can usually continue walking with mild medial knee pain as long as the activity doesn’t cause a limp or sharp, catching sensations. Gentle movement is beneficial because it maintains joint lubrication and prevents muscle wasting. If your pain levels exceed a 4 out of 10 on a standard pain scale, you should reduce your distance. Patients from Abingdon and Witney often find that a tailored walking plan from our specialists prevents further irritation.
How do I know if my medial knee pain is serious?
Your knee pain is considered serious if you experience joint locking, the knee “giving way,” or an inability to bear any weight. Significant swelling that appears within 2 hours of an injury also requires an immediate clinical assessment. These symptoms often suggest a grade 3 ligament tear or a displaced meniscus fragment. Our Oxford clinic provides diagnostic scans to give you a clear diagnosis within 48 hours, ensuring you start the correct recovery path.
What is the fastest way to relieve inner knee soreness?
The fastest way to relieve acute inner knee soreness is the POLICE protocol (Protection, Optimal Loading, Ice, Compression, Elevation) combined with professional clinical intervention. For persistent inflammation, a targeted corticosteroid injection can reduce pain within 24 to 48 hours. This allows you to begin rehabilitation exercises much sooner. We provide these advanced therapies to residents across Summertown and Headington to accelerate long-term recovery and restore comfort quickly.
Why does the inside of my knee hurt when climbing stairs?
Climbing stairs increases the load on your medial knee compartment by up to 3 times your body weight, which aggravates any underlying cartilage or tendon issues. This specific pain often points to Pes Anserine Bursitis or early-stage wear and tear. Strengthening the quadriceps and gluteal muscles can reduce this mechanical pressure by 15%. Our practitioners, easily accessible from Kennington and Marcham, focus on biomechanical retraining to make daily activities like climbing stairs pain-free again.
Do I need an MRI for medial knee soreness?
You don’t always need an MRI, as a thorough clinical examination by a specialist identifies the cause in 80% of musculoskeletal cases. We typically reserve MRI scans for complex symptoms or when conservative treatments haven’t produced results after 6 weeks. For many patients in Faringdon and Eynsham, an ultrasound scan at our clinic is a faster way to visualise soft tissue damage. This ensures a clear path to recovery without the long wait times often associated with hospitals.
Can physiotherapy fix a medial meniscus tear?
Physiotherapy is highly effective for treating degenerative or small traumatic medial meniscus tears without the need for invasive surgery. Research indicates that 75% of patients who choose a structured exercise programme achieve functional outcomes equal to those who undergo surgery. Our “one-stop setup” in central Oxford combines manual therapy with specific loading protocols. This approach helps restore knee function and prevents future injury, providing a reliable, evidence-based solution for long-term joint health.







