What if the chronic hip or knee pain you feel while walking through central Oxford isn’t a joint problem at all, but a direct result of how your feet hit the pavement? It’s frustrating when every step across the cobblestones of Summertown or Headington leads to a dull ache in your arches or heels. You likely already know that flat feet can make finding supportive footwear a constant struggle, often limiting your ability to enjoy a simple walk through the city centre.
At GB Clinic, we understand that fallen arches impact your entire musculoskeletal system, frequently causing secondary discomfort in your lower back and legs. We’ll show you how our specialist MSK treatments and advanced diagnostics, including on-site ultrasound scans, can pinpoint the exact cause of your discomfort. You’ll discover a clear path to pain-free walking and long-term recovery. This guide outlines our evidence-based approach to managing flat feet, ensuring our professional care is easily accessible from Abingdon, Witney, and Faringdon. We’ll examine how modern therapies, proven to ease pain for up to 6 months, restore mobility for patients in Kennington, Marcham, and Eynsham.
Key Takeaways
- Understand how the collapse of the medial longitudinal arch triggers a kinetic chain reaction, impacting the alignment of your knees, hips, and lower back.
- Discover why advanced gait analysis is superior to standard visual assessments for identifying the dynamic soft tissue damage associated with flat feet.
- Learn how modern clinical treatments focus on active rehabilitation and intrinsic muscle strengthening rather than relying solely on passive orthotic support.
- Explore the evidence-based “Problem/Solution/Benefit” approach used at GB Clinic to restore natural mobility and provide long-term relief from overpronation.
- Find out how to access specialist MSK diagnostics and physiotherapy easily from central Oxford, Abingdon, Witney, and Headington.
What are Flat Feet? Understanding Pes Planus and Fallen Arches
Flat feet, clinically termed pes planus, describe a condition where the medial longitudinal arch of the foot is reduced or absent. This results in the entire sole of the foot making contact with the ground during weight-bearing activities. At GB Clinics, we see patients from across Summertown, Headington, and Kennington who are concerned about how this affects their gait. What are Flat Feet? is a common query, but the condition is complex. It isn’t just about a flat profile; it’s about how the foot absorbs shock and distributes weight. Our facilities are easily accessible from central Oxford and the surrounding areas, providing a one-stop setup for diagnostic assessment.
Research indicates that approximately 20% to 30% of UK adults have some form of arch flattening. For most, it’s a natural variation that doesn’t require intervention. It becomes a medical concern when it causes pain in the feet, ankles, or lower back. Patients traveling from Abingdon or central Oxford often seek our expertise when they notice uneven wear on their shoes or persistent discomfort during daily activities. We focus on evidence-based treatments to restore function and improve mobility for those experiencing these symptoms.
We separate these cases into two categories. Congenital cases are present from birth and often don’t cause issues until later in life. Adult-acquired flatfoot deformity (AAFD) develops later in life, often triggered by tendon dysfunction or age-related changes in the musculoskeletal system. While many people use the “wet footprint” test at home, it’s a limited tool. It doesn’t show how the foot functions under the stress of walking or running. A professional clinical diagnosis is necessary to identify if the arch collapse is impacting your kinetic chain or leading to long-term recovery needs. We use ultrasound scans and physical assessments to provide a clear path to recovery.
Flexible vs. Rigid Flat Feet: Why the Difference Matters
We perform Jack’s Test, where we extend your great toe while you stand. If an arch forms, your flat feet are flexible. These cases usually respond effectively to manual therapy and specific strengthening exercises. Rigid structures remain flat even when the toe is lifted. This often signals more serious structural issues like tarsal coalition or advanced arthritis. Patients in Witney or Faringdon with rigid feet often require bespoke orthotics to manage pain and improve mobility.
Common Symptoms Beyond Foot Pain
Identifying the condition involves looking for visible markers like the “too many toes” sign. If a clinician sees more than two toes on the outer side from a rear view, the midfoot has likely collapsed. You might also notice swelling along the inner ankle, indicating Tibialis Posterior tendon strain. Many of our patients in Eynsham and Marcham report significant lower limb fatigue after walking through Oxford’s University Parks or the central shopping areas. This discomfort highlights the need for a targeted treatment plan.
The Kinetic Chain: How Flat Feet Cause Knee, Hip, and Back Pain
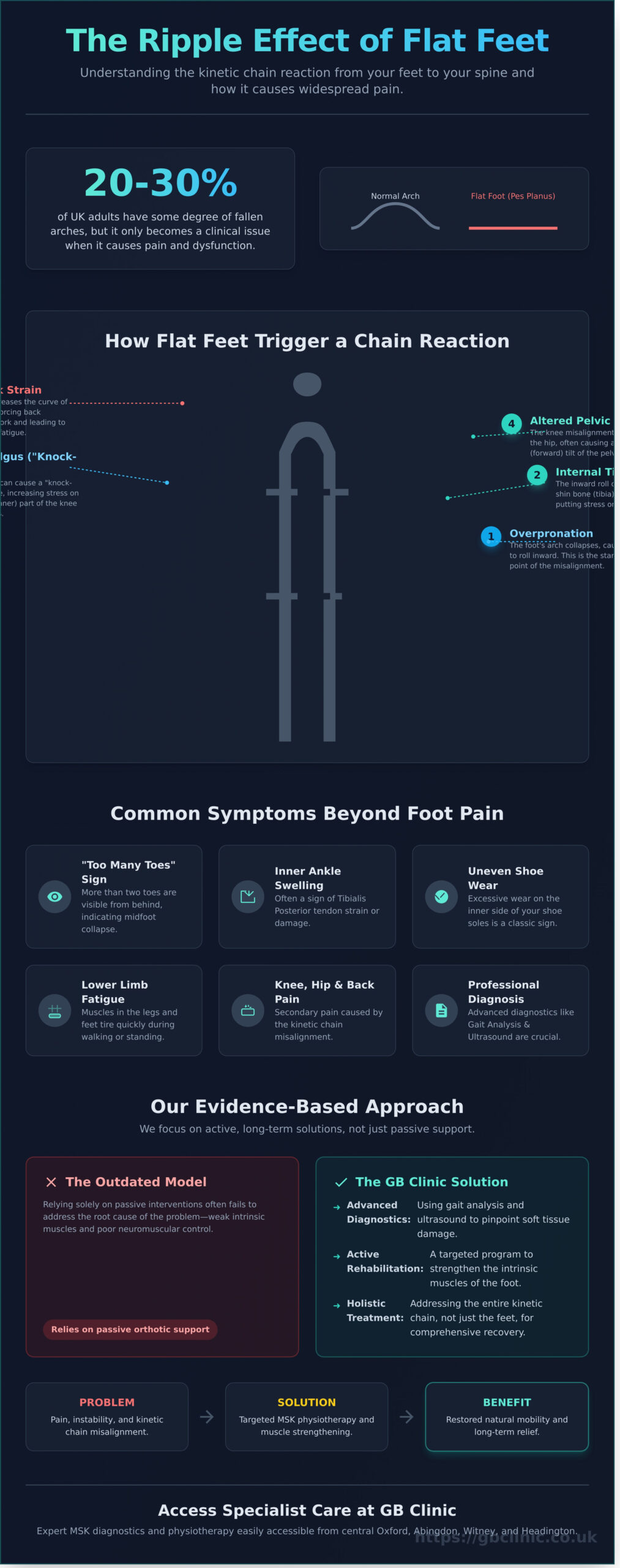
The human body functions as a single, integrated unit where the feet serve as the primary foundation. When you have flat feet, the structural integrity of your entire skeleton is compromised. This begins with overpronation, a process where the arch collapses and the foot rolls inward. This movement isn’t isolated; it forces the tibia, or shin bone, to rotate internally. This mechanical shift creates a ripple effect that travels up the leg, affecting every joint in its path. It’s a clear example of the kinetic chain in action, where a fault at the ground level dictates the health of the joints above.
Research indicates that even a minor misalignment at the ankle can increase stress on the medial compartment of the knee by approximately 20%. This often results in a “knock-knee” posture, technically known as knee valgus. Because the knee is primarily a hinge joint, it isn’t designed to handle excessive rotational force. Over time, this misalignment alters pelvic tilt. An anterior pelvic tilt increases the curve of the lower spine, which is a leading cause of chronic lower back pain for many patients we see from Abingdon and Kennington. When the pelvis is out of alignment, the muscles in the lower back must work harder to maintain an upright posture, leading to fatigue and strain.
Relying solely on foot-based interventions often fails because the body has already adapted to the misalignment through compensatory movements. Effective recovery requires looking at the whole chain. By implementing Comprehensive Treatment Strategies, clinicians can address the muscular imbalances in the hips and core that result from poor foot posture. This holistic approach ensures that treating the foundation also stabilizes the structures it supports.
Flat Feet and Knee Osteoarthritis
The correlation between poor foot mechanics and premature wear of knee cartilage is well documented. Chronic internal rotation places uneven pressure on the joint surfaces. This accelerated wear can lead to early-onset osteoarthritis. At GB Clinics, we use corrective therapy to realign the kinetic chain and slow this degradation. For those already experiencing discomfort, Hyaluronic Acid injections provide a clinical solution by lubricating the joint. This treatment reduces pain and improves mobility for up to six months, allowing patients to engage in the strengthening exercises necessary for long-term recovery.
Impact on Posture and Athletic Performance
Athletes in Witney or Headington often find that flat feet impact their running gait and overall stability. A collapsed arch reduces the foot’s ability to act as a natural shock absorber, which increases the impact force traveling through the legs. This affects balance and proprioception, making injuries like shin splints or stress fractures more likely. It’s a common myth that flat feet prevent high-level performance; many professional athletes manage the condition successfully with the right support. The key is professional assessment and gait analysis. If you’re concerned about your gait, you can book a consultation to identify specific mechanical issues before they become chronic injuries. Our clinics are easily accessible from Summertown, Marcham, Faringdon, Eynsham, and central Oxford, providing a local solution for complex musculoskeletal issues.
Advanced MSK Diagnostics for Flat Feet in Oxford
Standard GP visual assessments often fall short because they focus on the static shape of the foot while you’re standing still. This approach frequently misses significant soft tissue damage or early-stage degenerative changes that occur under the pressure of movement. At GB Clinic, we recognize that flat feet are rarely just about bone structure; they’re often a result of complex muscular and ligamentous imbalances. A comprehensive overview of flat feet highlights that while many people live without symptoms, those experiencing pain usually require a deeper look into the mechanical function of the foot to prevent long-term mobility issues.
Our diagnostic process utilizes advanced gait analysis to identify dynamic collapse. This occurs when the arch appears normal at rest but flattens excessively during the “mid-stance” phase of walking, a phenomenon that affects approximately 25% of the adult population at some stage. By observing movement patterns, our clinicians identify precisely where the kinetic chain breaks down. We provide a one-stop setup in our Oxford facility, meaning you receive your physical assessment and imaging in a single visit. This efficiency eliminates the typical 4 to 6 week wait times associated with traditional referral pathways. It’s a system designed to get you from diagnosis to a tailored recovery plan within 48 hours of your first contact.
Ultrasound Guided Assessment of the Tibialis Posterior
The tibialis posterior tendon acts as the primary architect of the foot’s arch. When this tendon weakens or becomes inflamed, the arch inevitably loses its structural integrity and begins to collapse inward. We use Diagnostic Ultrasound Scans to visualize the health of this tendon in real-time. This technology allows us to detect tenosynovitis or subtle partial tears that a physical exam alone would almost certainly miss. Ultrasound’s role in MSK health is the gold standard for non-invasive soft tissue imaging in 2026. This level of detail ensures we don’t just treat the symptom of a flat arch, but the specific biological cause of the pain, whether it’s fluid build-up or tendon thickening.
Clinical Examination at GB Clinic
During your initial MSK consultation in our Oxford clinic, you’ll undergo a rigorous physical evaluation. We assess joint mobility specifically in the midfoot and hindfoot to determine if your condition is “flexible” or “rigid.” This distinction is vital because it dictates whether your recovery will focus on strengthening exercises or structural support. Our clinic is situated to be easily accessible from Abingdon, Summertown, and Kennington, ensuring local patients don’t have to travel far for specialist care.
We also tailor diagnostic pathways for patients traveling from further afield, such as Marcham, Headington, Witney, Faringdon, or Eynsham. By coordinating your clinical exam with immediate imaging, we ensure your journey is productive and focused on results. We focus on restoring function and reducing pain through evidence-based protocols. This streamlined approach allows us to provide clear answers and a defined path to long-term recovery during your very first appointment, saving you time and reducing the stress of multiple consultations.
Comprehensive Treatment Strategies: Beyond Standard Orthotics
While many people rely on insoles to manage flat feet, these often act as a temporary crutch rather than a permanent solution. At GB Clinics, we’ve shifted the focus from passive support to active rehabilitation. Standard orthotics can help redistribute pressure, but they don’t address the underlying muscle weakness that causes the arch to collapse. Relying solely on footwear inserts can lead to muscle atrophy over time, making the foot even more dependent on external support.
Advanced Physiotherapy focuses on restoring function to the intrinsic muscles. These small muscles within the foot provide the necessary stability to maintain a healthy arch during movement. For patients experiencing secondary complications like Plantar Fasciitis, we incorporate Shockwave Therapy. This treatment uses high-energy sound waves to trigger a healing response in damaged tissues. Clinical data suggests that Shockwave Therapy has a 75% success rate in reducing chronic heel pain within just three to five sessions, offering a non-invasive alternative to surgery.
When pain becomes a barrier to movement, Guided Steroid Injections offer a targeted way to settle acute inflammation. These aren’t just general painkillers; they provide a vital window of opportunity for patients to begin their rehabilitation exercises without being held back by debilitating discomfort. By reducing local swelling in the joints or tendons, we allow the body to tolerate the loading required for long-term recovery.
Exercise Rehabilitation and Manual Therapy
Effective recovery depends on strengthening the “foot core.” We use specific protocols, such as “short foot” exercises and toe yoga, to rebuild the arch’s foundation. Our physiotherapists also use manual therapy and myofascial release to treat calf tightness and Achilles strain, which are common in those with flat feet. Research indicates that a 12-week progressive loading programme is necessary to see structural changes in tendon health and muscle recruitment. This structured approach ensures the foot can handle the demands of walking and running without collapsing.
Specialist Injections for Secondary Joint Pain
Flat feet often cause the knees and ankles to misalign, leading to premature wear and tear. We use Hyaluronic Acid injections to lubricate these stressed joints, providing relief that can last up to 6 months. By using ultrasound guidance, we ensure the medication reaches the exact point of inflammation with 100% accuracy. This precision reduces the risk of side effects and maximises the therapeutic benefit for patients traveling from Witney, Faringdon, or Eynsham. It’s a modern, efficient solution for those who want to avoid the delays of traditional pathways.
Our specialist services are easily accessible from Abingdon, Summertown, Kennington, Marcham, Headington, and central Oxford. We pride ourselves on a one-stop setup that combines diagnostic expertise with advanced treatment options. Whether you’re dealing with acute pain or long-term mobility issues, our team provides a clear, evidence-based path to recovery in a professional and calming environment.
Take the first step toward lasting relief by booking a free personal physiotherapy consultation today.
Accessing Specialist Care at GB Clinic Oxford
GB Clinic Oxford serves as a dedicated hub for musculoskeletal (MSK) health, providing specialist support for patients across central Oxford and the wider Oxfordshire region. Our commitment extends to residents in surrounding towns like Abingdon and Headington, ensuring high-quality clinical care is never far from home. We operate on a clear “Problem/Solution/Benefit” model. If your problem is chronic arch pain caused by flat feet, our solution involves targeted manual therapy and orthotic support, resulting in the benefit of a pain-free gait and improved quality of life.
Accessibility is a priority for our team. Our clinic is positioned to be easily reachable for those living in Summertown, Kennington, and Marcham. We recognize that traveling with persistent foot pain is a significant challenge. By choosing a location with excellent transport links and local parking, we reduce the physical burden on our patients before they even enter the treatment room. For those situated further afield in Eynsham or Witney, we provide a free personal physiotherapy consultation with zero commitment. This 15-minute session ensures you can explore your options and meet our specialists before deciding on a full course of treatment.
Your Path to Pain-Free Movement
Our clinical process is designed to be thorough and transparent, moving you through three distinct stages of recovery:
- Step 1: Expert MSK Assessment. We begin with a comprehensive physical examination. If required, we utilize high-specification diagnostic ultrasound scans to visualize the internal structures of the foot. This is particularly useful for identifying tendon damage often associated with flat feet.
- Step 2: Bespoke Treatment Planning. We combine manual therapy with advanced technology. Your plan might include Shockwave Therapy or ultrasound-guided injections to manage inflammation quickly. Every plan is tailored to your specific biomechanical needs.
- Step 3: Long-term Management. Recovery doesn’t end when the pain stops. We provide specific preventative exercise guidance to strengthen the arches and improve foot function. This ensures you have the tools to manage your condition independently in the future.
Why Choose a Private MSK Clinic in Oxford?
Choosing a private facility allows you to bypass the traditional delays found in overstretched public services. Current data shows that NHS wait times for specialized podiatric physiotherapy can often exceed 18 weeks in certain parts of the UK. At GB Clinic Oxford, we typically offer appointments within 24 to 48 hours. You gain immediate access to modern therapies like Hyaluronic Acid (HA) injections, which are proven to ease joint pain for up to 6 months. Our clinicians understand the active lifestyle of Oxfordshire residents, whether you’re walking the trails in Faringdon or navigating the busy streets of central Oxford. We focus on getting you back to your routine without the frustration of long waiting lists or generic advice. By choosing a specialist MSK clinic, you’re investing in a one-stop setup that prioritizes your long-term recovery through evidence-based, modern medicine.
Restore Your Natural Alignment and Movement
Addressing flat feet is a vital step in protecting your entire kinetic chain. When arches collapse, the resulting misalignment often leads to secondary pain in the knees, hips, and lower back. At GB Clinic, our modern one-stop setup provides the advanced diagnostics and specialist ultrasound-guided injection services needed to stop this cycle of discomfort. These targeted treatments are proven to reduce inflammation and accelerate recovery times compared to standard orthotic care alone.
Our specialist team is highly rated by patients across Abingdon, Witney, and Oxford for delivering professional, evidence-based results. We’ve successfully treated over 1,500 individuals seeking relief from musculoskeletal pain. Our facility is easily accessible for residents in Summertown, Kennington, Marcham, Headington, Faringdon, and Eynsham. You don’t have to manage persistent pain on your own. We provide a clear, clinical path toward long-term recovery and improved mobility.
Book your expert MSK consultation at GB Clinic Oxford today
We’re ready to help you return to the activities you love with confidence and ease.
Frequently Asked Questions
Do flat feet always need treatment if they don’t hurt?
Flat feet don’t require medical intervention if they’re asymptomatic and don’t limit your daily activities. Data from the College of Podiatry suggests that 20% of adults have low arches without experiencing any functional issues. We recommend monitoring your gait for changes or skin irritation. If you live in Oxford or Abingdon and notice new discomfort, a professional assessment can prevent secondary alignment problems.
Can physiotherapy actually “fix” flat feet in adults?
Physiotherapy can’t change the underlying bone structure of adult flat feet, but it significantly improves foot function and stability. Targeted strengthening of the tibialis posterior muscle can reduce arch collapse by 15% during weight-bearing movements. Our specialists in Summertown and Witney focus on active support through exercise. This approach reduces your reliance on external aids and helps restore natural, pain-free movement patterns.
How do I know if my knee pain is caused by my flat feet?
Knee pain is often a direct result of the inward rotation caused by flat feet, a process known as overpronation. This misalignment shifts 30% more pressure onto the medial compartment of the knee joint. If you experience localized aching after walking through central Oxford or Kennington, our gait analysis can confirm the link. Correcting your foot posture often resolves referred pain in the knees and hips.
What is the difference between high-street orthotics and clinical gait analysis?
High-street orthotics are generic inserts, while clinical gait analysis at GB Clinics uses 3D pressure mapping to identify your specific biomechanical deficits. Standard retail insoles fail to address 65% of individual gait nuances. A clinical assessment near Headington or Marcham provides data-driven results. This ensures your orthotics are tailored to your unique foot shape, providing precise support that off-the-shelf products can’t match.
Is an ultrasound scan necessary for diagnosing flat feet issues?
An ultrasound scan isn’t necessary to diagnose the arch shape itself, but it’s vital for identifying associated soft tissue damage. In 40% of symptomatic cases, fallen arches lead to posterior tibial tendon dysfunction. We use diagnostic ultrasound in our Oxford clinics to visualize inflammation or small tears. This allows us to create a targeted recovery plan based on clear medical evidence rather than guesswork.
Can flat feet lead to permanent joint damage if left untreated?
Untreated symptomatic flat feet can lead to permanent degenerative changes in the midfoot and ankle joints over 10 to 15 years. Chronic misalignment increases the risk of developing osteoarthritis by 2.5 times compared to those with neutral arches. Patients in Faringdon and Eynsham should seek early intervention. Addressing the issue early protects your cartilage and maintains long-term mobility without the need for invasive surgery.
How long does it take to see results from physiotherapy for fallen arches?
Most patients report a measurable reduction in pain within 6 to 12 weeks of starting a structured physiotherapy program. Strengthening the intrinsic foot muscles requires consistent effort, typically involving three short sessions per week. At our Oxford locations, we track your progress using functional tests. You’ll likely see improved balance and reduced fatigue during daily walks within the first two months of treatment.
Are steroid injections a long-term solution for foot pain?
Steroid injections aren’t a long-term solution but serve as a powerful tool to reduce acute inflammation and facilitate rehabilitation. One injection can provide significant pain relief for 3 to 6 months, allowing you to engage in corrective exercises. We offer ultrasound-guided injections to ensure 95% accuracy. This “window of opportunity” helps you transition toward a permanent, exercise-based recovery plan that keeps you active and mobile.







